How cities are prioritizing equity in their vaccine rollout efforts
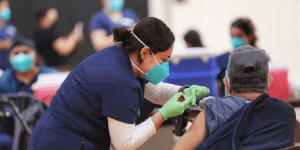
To increase the pace of COVID-19 vaccinations in Latinx communities, the city of Long Beach, Calif., is partnering with community groups to host mobile clinics like this one last month. (City of Long Beach photo)
The Latinx neighborhoods Councilwoman Mary Zendejas represents in Long Beach, Calif., have been hit hard by COVID-19. So when Zendejas saw that residents in her district were getting vaccinated at much lower rates than people in other parts of the city, she got to work.
She mobilized a task force she created earlier in the pandemic—called Latinos Contra COVID—which includes several community organizations and city Health Department and Latinx city staff members. They then set up a series of mobile vaccination clinics aimed at Spanish-speaking residents who’ve been hard to reach, such as seniors who might not be comfortable with online signups.
“We knew that there were a lot of abuelitas and abuelitos, tios and tias, who were not technology-savvy enough to log in and register for their vaccine,” Zendejas said. “What the community groups did is reach out the old-fashioned way: Calling them, walking around and talking to them. They were able to get them on the list and get them vaccinated.”
These clinics have now vaccinated about 1,000 people, Zendejas said. That includes a number of undocumented residents who’ve been reassured that they won’t be asked questions about immigration status. And while vaccinations in Long Beach are still lagging among residents who identify as Hispanic or Latino according to the city’s data dashboard, Zendejas said the mobile clinics are making a difference. “It’s definitely moving the needle,” she said. “It’s really slow, but it’s moving in the right direction. And that’s what we need.”
Clinics like these are just one response to a pressing problem faced by cities across the country. After a year in which COVID-19 took an outsized toll on people of color, the vaccine rollout is following an alarmingly similar trajectory. National data show disproportionately low rates of vaccination among African-Americans and Hispanics—although data are known for only about half of the people who’ve received at least one shot. Data dashboards from most cities that have them are showing the same patterns.
Bloomberg Philanthropies has partnered with the U.S. Conference of Mayors to provide critical guidance to city leaders for ensuring that the vaccine rollout is both equitable and effective. These resources include evidence-based messages for encouraging vaccination; a guide to public engagement and communications; data and monitoring strategies; and an overview on the role mayors can play.
In Long Beach, which has been hailed as a national model for the vaccine rollout, Mayor Robert Garcia told Bloomberg Cities that equity is a major focus. It’s complicated, however, by the emphasis on vaccinating older residents first. Most of the city’s 65-plus population is White, said Garcia, who lost both his mother and stepfather to COVID last year. That makes it critical to deploy targeted approaches aimed at reaching communities of color.
In Long Beach, that means going well beyond the mass vaccination site at the city’s convention center. There are additional mobile clinics serving the city’s Cambodian community, and more set up in Black churches in partnership with the NAACP. “To really move equity in the direction you want,” Garcia said, “jurisdictions that have diverse populations have to push really, really hard to get those numbers moving.”
Garcia highlighted some other ways that Long Beach is prioritizing equity. Early on, the city expanded vaccine eligibility to include food and grocery workers, a group that includes more people of color whose work environments put them at high risk of COVID. The city has been liberal about vaccinating caretakers and family members who bring in seniors to be vaccinated, on the grounds that multigenerational households are common in the Latino community. And Garcia said he does a lot of press appearances in Spanish, the most commonly spoken language in the city after English, “just so that people hear me in their own language.”
[Find data-driven messages in English and Spanish to help increase vaccine uptake here]
Long Beach last week also became the first jurisdiction in California to prioritize people with physical and mental disabilities for vaccination. That was something Zendejas, who uses a wheelchair, was glad to see. “The disability community has been overlooked” in the COVID-19 vaccine rollout, she said.
Chrissie Juliano, head of the Big Cities Health Coalition, said it can sometimes feel like the vaccine rollout is a matter of speed versus equity—especially when supply remains scarce. But it doesn’t have to be that way, she said. Speed and equity can go together if city leaders are intentional about prioritizing equity and engage local communities in making hyper-local decisions. “The struggle between speed and equity is a challenge,” Juliano said. “Clearly we need both. And the leadership and expertise we see in many big cities can work to meet both goals”
Here are some ways that cities across the U.S. are innovating to do just that.
Targeting vulnerable communities
Chicago has targeted 2,000 shots a week to 15 high-need neighborhoods based on a vulnerability index that takes cumulative COVID burden, occupational risks, and other factors into account. In these areas, any residents age 16 and up—regardless of age, underlying conditions, or other common criteria—can get a shot at mobile clinics held in the neighborhood.
As a result, the portion of the city’s vaccine supply going to Black and Latinx residents each week went from 18 percent at the beginning of the rollout to more than 50 percent in recent weeks. “Equity is not only part of our COVID-19 strategy,” Mayor Lori Lightfoot said when rolling out the plan called Protect Chicago Plus. “Equity is our strategy.”
Other cities, such as Baltimore, San Francisco, and Washington, D.C., are trying similar approaches, prioritizing vaccinations in certain ZIP codes in hopes of producing a more equitable outcome.
Stepping up outreach through community partnerships
Cities are leaning on community organizations, churches, and other trusted partners to host mobile clinics and lead outreach efforts. The partnerships are critical for overcoming distrust toward government or vaccines, and also for providing pathways to vaccination that don’t lead through clunky online signup forms.
For example, Detroit has partnered with Black churches for its “Senior Saturdays” vaccination drive. The clinics, now administering 2,000 shots per week, are one reason why 82 percent of doses allocated to the Detroit Health Department and administered to city residents have gone to Black residents. “We are working closely with our faith-based leaders to bring the vaccine to seniors, meeting them close to home,” said Detroit’s chief public health officer, Denise Fair.
In Long Beach, Councilwoman Zendejas said the city’s progress so far would be impossible without partnerships. “Our community-based organizations have been working with the Latino community for years,” she said. “We really need to lean on them to help us get all of our Latino residents vaccinated.”
[Get our guide to public engagement around vaccines here]
Using data to guide the effort
In the pandemic’s early days, testing data tended to mask the racial and ethnic disparities that were playing out in COVID cases. The same is true with vaccination, unless leaders push hard to make sure data on race, ethnicity, age, ZIP code, and other factors are collected and reported. In Chicago, Public Health Commissioner Allison Arwady signed an order requiring providers to collect and report this data. Long Beach is reporting race and ethnicity data on all but 4 percent of its vaccinations.
“We’re very data-driven,” Long Beach Mayor Garcia said. “That was really important for us from day one. It allows us to make better decisions.”
[Get our guide to vaccine data and monitoring strategies here]
Making signing up for a vaccine easier
For many people, the biggest barrier to vaccination has been finding out where to get it and the mechanics of making an appointment. Washington, D.C., is addressing this in part through its “Senior Vaccine Buddies” program. Outreach teams of city employees are going door-to-door in vulnerable areas to help people age 65 and older schedule their appointments. In Youngstown, Ohio, where the City Health District was struggling to keep up with phone calls, emails, and text messages from residents, the city launched an online scheduling tool that allows residents to book vaccine appointments in less than a minute.
In Anchorage, Alaska, the city’s innovation team came up with a fix for a common problem for people across the country: The need to check with many different public and private clinics and pharmacies to find one with an available appointment. They created a website that shows every available appointment and updates every two minutes.
The team has scaled up the tool to include other cities in Alaska—making it, essentially, the vaccine finder for the entire state. The state’s main vaccine call center uses it to connect people to appointments, and both the state health department and the state’s largest newspaper have embedded the tool on their websites. (The tool can be easily repurposed to work in other states as well—the i-team has made the software code freely available here.)
“The pandemic prepared us for knowing that this is going to be chaotic and we have to be really nimble,” said Ben Matheson, the i-team’s data analyst, who designed the tool. “We can change things really fast, and that’s been our secret sauce.”